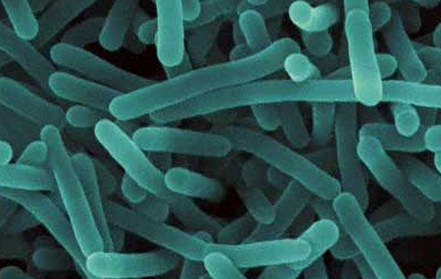
Foodborne pathogens, such as bacteria and parasites in consumable goods, can result in illnesses and deaths, wreaking havoc on residents of states and countries. The companies at fault often face severe damage to their reputation as people fear that continuing to do business with a brand is not safe. Moreover, if the affected enterprises do not take decisive steps to prevent the problem from happening again, they may receive substantial fines or closure orders.
Statistics from the U.S. federal government indicate that there are approximately 48 million cases of foodborne illnesses in the American food supply each year. Fortunately, there are proven steps that production plant managers can take to minimize the risk of foodborne pathogens. Being familiar with the preventative measures, and taking steps to implement them prevents catastrophes.
Engage with Suppliers about Their Efforts to Kill or Reduce Foodborne Pathogens
Foodborne pathogens can enter a production plant on items like fresh produce received from farm suppliers. Agricultural professionals commonly use chlorine to decontaminate goods before shipping them. However, researchers used a chlorine solution on spinach leaves to assess its effectiveness in killing common types of bacteria. The team discovered that, even after chlorine exposure, some bacteria remained viable but undetectable by industrial methods.
Foodborne pathogens can originate at farms for other reasons, too. Failing to take the proper precautions during animal slaughter can introduce contaminants into meats that end up in food production facilities. Water impurities can also pose dangers.
All production plants should regularly communicate with suppliers about the actions they take against foodborne pathogens. Food safety is a collective effort. Practicing it means following all current guidance, plus updating methods if new research justifies doing so. If suppliers resist doing what’s in their power to stop foodborne pathogens, they must realize they’re at risk for severing profitable relationships with production plants that need raw goods.
Consider Using Sensors to Maintain Safe Conditions
The Internet of Things (IoT) encompasses a massive assortment of connected products that benefit industries and consumers alike. One practical solution to enhance food safety in a production plant involves installing smart sensors that detect characteristics that humans may miss.
For example, the USDA published a temperature safety chart that explains what to do with food after a power outage. Most items that people typically keep in refrigerators become dangerous to eat if kept above 40o F for more than two hours.
Food production plants typically have resources like backup power to assist if outages occur. But, imagine a cooler that appears to work as expected but has an internal malfunction that keeps the contents at incorrect temperatures. IoT sensors can help production plant staff members become immediately aware of such issues. Without that kind of information, they risk sending spoiled food into the marketplace and getting people sick.
Researchers also developed a sensor-equipped device that detects the effectiveness of hand washing efforts. In a pilot program involving 20 locations, contamination rates decreased by 60% over a month. Most restrooms at food preparation facilities remind people to wash their hands before returning to work. What if a person takes that action, but not thoroughly enough? Specialty sensors could reduce that chance.
Install Germicidal Ultraviolet Lights
With much of the world on lockdown due to the COVID-19 pandemic, many people want to know if germicidal ultraviolet lights could kill the novel coronavirus. Researchers lack enough information to answer that question definitively. They do know, however, that germicidal ultraviolet lights kill up to 99.99% of bacteria and pathogens.
Plus, these lights are particularly useful in food production because they get the job done without harsh chemicals that could make products unsafe. Ultraviolet lights can damage the skin and eyes, so you must only run them when there are no humans in the room. However, it’s immediately safe to enter the environment after switching the lights off.
These specialized light sources do not eliminate the need for other food safety measures. Think about implementing them as another safeguard against adverse consequences.
Teach Workers about Safe Practices
Food contamination risks exist at numerous points along the supply chain. Mishandling is a major culprit that could make several parties partially responsible for a foodborne pathogen problem. For example, if a person does not wear the proper gear when handling food or stores items intended for raw consumption in places where meat juices touch them, either of those things and many others could cause issues with foodborne pathogens.
As you inform employees about which procedures to take to manage the risks, emphasize that everyone has an essential role to play in keeping products free from contaminants. If workers make ready-to-eat foods, such as packaged sandwiches, ensure they understand how to avoid the cross-contamination that happens when reusing cutting boards or utensils without washing them first.
The FDA requires domestic and foreign food facilities to analyze and mitigate risks. Employee training is not the sole aspect of staying in compliance, but it’s a major component. If a person makes a mistake due to improper or nonexistent training, that blunder could have significant financial ramifications for a food production facility.
Widely cited statistics indicate that food recall costs average more than $10 million, which is a staggering figure in itself. It doesn’t include litigation costs incurred when affected individuals and their loved ones sue companies, or the expenses associated with efforts to rejuvenate a brand and restore consumer confidence after people decide to take their business elsewhere.
Ensuring that workers receive the necessary training may be especially tricky if a human resources professional hires a large batch of temporary employees to assist with rising seasonal demands. If a higher-up tells them that time is of the essence and the new workers must be ready to assume their roles on the factory floor as soon as possible, training may get overlooked. When that happens, the outcomes could be devastating. Efficiency should never get prioritized over safety.
Stay Abreast of Emerging Risks
Besides doing your part to curb well-known threats that could introduce foodborne pathogens, spend time learning about new problems that you may not have dealt with before.
For example, scientists have not confirmed the origin of COVID-19. However, since early evidence suggested live animal sales and consumption may have played key roles, Chinese officials cracked down on the wildlife trade and imposed new restrictions on what was largely an unregulated sector cloaked in secrecy.
Much remains unknown about COVID-19, and it’s but one virus for food producers to stay aware of and track as developments occur. The ongoing pandemic is a sobering reminder not to blame specific groups or ethnicities, and to avoid jumping to hasty conclusions. It’s good practice to dedicate yourself to learning about any production risks that could introduce foodborne pathogens. Read reputable sources, and don’t make unfounded assumptions.
A Collective and Constant Effort
There is no single way to combat all sources of foodborne pathogens. Instead, anyone involved in food production or supply must work diligently together and know that their obligation to prevent issues never ceases.